What is a Cataract and How Does it Develop?
Cataract is an eye condition that affects millions of people globally. It develops when the eye’s lens becomes cloudy, leading to blurred vision and if left untreated, potential vision loss. cataracts can develop at any age but are commonly associated with aging. The lens of the eye, located behind the iris and pupil, plays a crucial role in focusing light onto the retina, enabling clear vision. This lens is primarily made up of water and protein.
Over time, the protein in the lens can clump together, forming cloudy areas known as cataracts. These cloudy areas disrupt the passage of light through the lens, resulting in blurred or dim vision. Cataracts can develop slowly over years or progress rapidly, depending on various factors such as age, genetics, and lifestyle. Cataracts can vary in severity and progression, with two primary classifications: Mature and Immature cataracts.
What is a Mature and Immature Cataract?
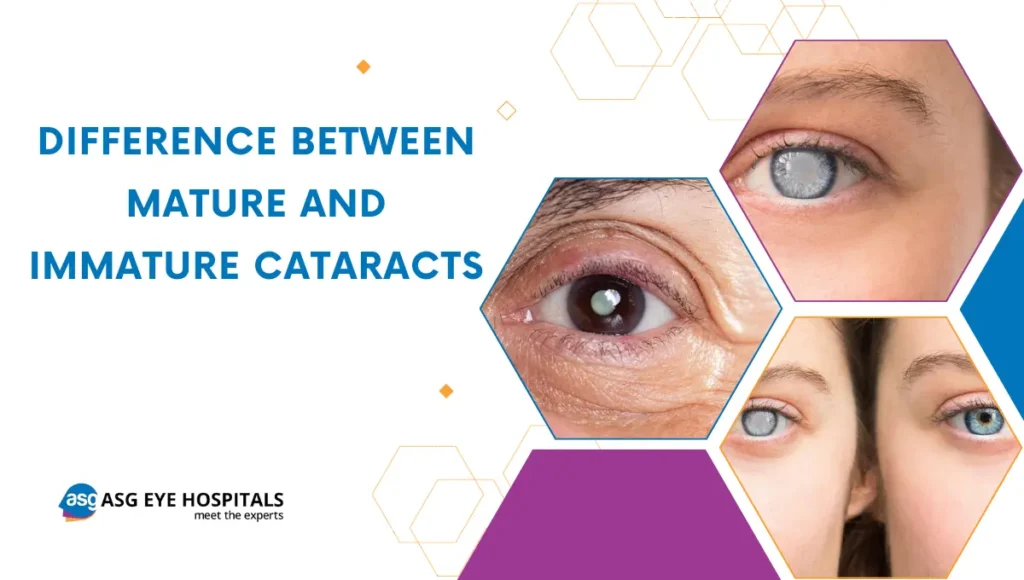
Mature cataracts refer to advanced stages of cataract development where the cloudiness of the lens has significantly progressed, causing noticeable vision impairment.
Immature cataracts are early-stage developments characterized by minimal cloudiness or opacity of the lens. While vision may be slightly affected, it is often not as pronounced as mature cataracts.
Some Key Features of Mature Cataracts
- Severe Vision Impairment: In mature cataracts, the cloudiness of the lens is extensive, resulting in significant vision impairment. Patients may experience blurred vision, double vision, difficulty seeing in low light conditions, or even complete loss of vision in the affected eye.
- Opaque Appearance: The affected lens appears opaque or milky white, obscuring the passage of light to the retina.
- Increased Risk of Complications: Mature cataracts can lead to various complications if left untreated, such as increased intraocular pressure (glaucoma), inflammation, or even retinal detachment. Prompt medical intervention is essential to prevent further vision loss and complications.
- Impact on Daily Activities: Due to the significant vision impairment associated with mature cataracts, patients may struggle with daily activities such as reading, driving, or recognizing faces. Quality of life can be substantially affected, increasing dependence on others for assistance.
Some Key Features of Immature Cataracts
- Mild to Moderate Vision Changes: vision changes in immature cataracts are typically mild to moderate. Patients may experience slight blurriness, glare sensitivity, or difficulty seeing in bright light.
- Partial Cloudiness: The lens may exhibit partial cloudiness or discoloration, affecting only a portion of the visual field. This partial opacity may not significantly impact overall vision but can cause discomfort or visual disturbances.
- Slower Progression: Immature cataracts tend to progress more slowly than mature cataracts. While they may worsen over time, the rate of deterioration varies among individuals and depends on factors such as age, underlying health conditions, and lifestyle choices.
- Potential Reversibility: In some cases, early-stage cataracts may be reversible or manageable through lifestyle modifications, dietary changes, or prescription eyewear. Regular eye examinations are crucial for monitoring progression and determining the most appropriate action.
Stages of Development of Cataract
Stage 1. Early cataract – This is the beginning stage of a cataract, in which the eye lens is clear but minor changes can be seen that are hardly noticed such as difficulty in focusing, slightly blurry vision, and headaches.
Stage 2. Immature cataract – In this stage, cataracts progress and become cloudier. Vision may become noticeably blurred to seeing an object, especially in low lights. Other symptoms may include seeing colorless vividly, difficulty reading small print, and experiencing halos and glare around lights.
Stage 3. Mature cataract – In this stage, the cataract is fully developed, and vision abnormalities become more severe. The lens becomes significantly clouded, obscuring vision and causing substantial visual disturbances. Individuals with mature cataracts may experience significant difficulty performing routine tasks such as driving, reading, or recognizing faces. Vision may be severely blurred or obscured, leading to a marked decline in overall visual function.
Stage 4 Hypermature cataract- In some cases, if left untreated for an extended period, a mature cataract may progress to a hypermature stage. During this stage, the lens may shrink and become wrinkled or folded, causing further distortion of vision. Hypermature cataracts can lead to complications such as inflammation or an increased risk of secondary issues like glaucoma or retinal detachment. Prompt treatment is essential to prevent these complications.
Treatment Options for Mature and Immature Cataracts
Immature Cataracts:
In the early stages of cataracts, especially if vision is only minimally affected, your doctor may recommend regular monitoring of your symptoms without immediate surgical intervention. You may be advised to use brighter lighting, update your eyeglass prescription, and minimize glare to help manage symptoms.
If your vision is affected by an immature cataract, your eye doctor may prescribe glasses or contact lenses to help improve your vision temporarily. However, these measures won’t prevent the cataract from progressing, and surgery may eventually be needed as the cataract matures.
Mature Cataracts:
Cataract Surgery (Phacoemulsification): Cataract surgery is the standard treatment for mature cataracts. During the procedure, the cloudy lens is removed and replaced with an artificial intraocular lens (IOL). Phacoemulsification is the most common technique used, where the surgeon uses ultrasound energy to break up the cataract into small pieces, which are then removed through a small incision in the eye. This surgery is usually performed under local anesthesia and is considered safe and highly effective.
Manual Extracapsular Cataract Extraction (ECCE): In cases where phacoemulsification may not be suitable, such as with very dense cataracts, manual ECCE may be performed. This involves removing the cataract through a larger incision, along with the lens capsule, and replacing it with an IOL.
Intraocular Lens (IOL) Options: There are various types of IOLs available, including monofocal, multifocal, and Toric lenses. Your surgeon will discuss the most suitable option based on your visual needs and lifestyle preferences.
Posterior Capsule Opacification (PCO) Treatment: Sometimes, after cataract surgery, a condition called posterior capsule opacification (PCO) can occur, where the membrane behind the IOL becomes cloudy, causing vision to become blurred again. This can be treated with a simple laser procedure called YAG laser capsulotomy, which clears the cloudiness and restores clear vision.
Conclusion
In summary, cataracts are a common age-related eye condition characterized by the clouding of the lens. Mature cataracts represent advanced stages of development, leading to severe vision impairment and increased risk of complications. In contrast, immature cataracts are early-stage developments with milder symptoms and slower progression. Understanding the difference between mature and immature cataracts is essential for timely diagnosis, treatment, and vision preservation. If you experience any changes in your vision, consult an eye care specialists for evaluation and appropriate management.