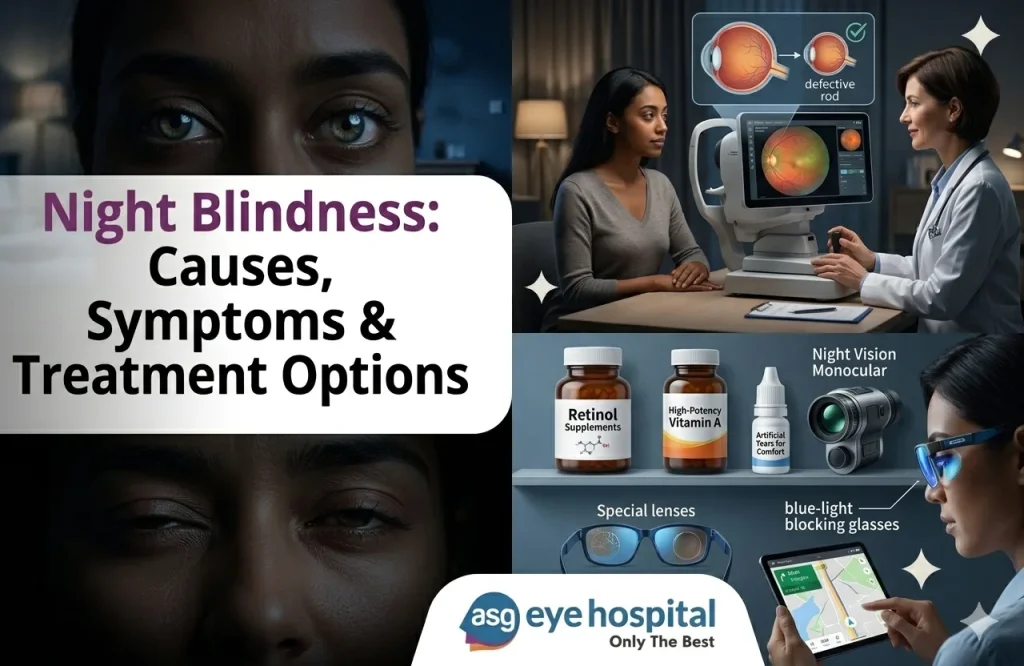
Most people notice it first when driving. Oncoming headlights scatter into a blur. The road beyond the beam becomes harder to read. Street signs that were clear a year ago now need a second look. It may be attributed to tiredness, or ageing, or not having updated a glasses prescription.
Difficulty seeing at night is common and frequently dismissed. But poor night vision is a symptom, not an inevitability, and its cause determines both the urgency and the treatment. Understanding what is behind it is the starting point.
What night blindness actually means
Night blindness, medically called nyctalopia, is not blindness in the conventional sense. It refers specifically to difficulty seeing in low-light conditions: dim rooms, dusk, poorly lit streets, or during the transition from a bright space to a dark one. Daytime vision is usually unaffected in most forms of the condition.
The retina contains two types of photoreceptor cells: cones for colour and daylight vision, and rods for dim light. Rod cells depend on a photopigment called rhodopsin, which regenerates in darkness. When any part of this system is impaired -by nutritional deficiency, structural disease, or optical factors -the result is difficulty seeing at night.
Night blindness symptoms and how they present
Night blindness symptoms are often noticed gradually rather than as a sudden change. The most consistent presentations include:
- Difficulty reading road signs, registering faces, or seeing obstacles in dimly lit environments
- Prolonged adjustment time when moving from a bright to a dark space -the normal dark adaptation process takes longer than expected
- Increased sensitivity to glare, particularly from oncoming headlights at night
- A reduction in peripheral vision in dim light, sometimes described as a narrowing or tunnel effect
- Stumbling over objects or misjudging steps when the lighting is poor
The pattern of symptoms often contains useful diagnostic information. Night blindness symptoms that include a progressive narrowing of peripheral vision, particularly in someone with a family history of eye conditions, suggest a different underlying cause than night blindness that came on over weeks alongside dry eyes and skin changes.
Night blindness causes and the spectrum from simple to serious
Understanding the cause is what determines whether a correction, a supplement, or a specialist referral is the appropriate next step.
Vitamin A deficiency is among the most correctable causes worldwide. Rhodopsin synthesis depends directly on Vitamin A, and when absorption is impaired through conditions like coeliac disease, Crohn’s disease, or post-bariatric surgery, rod function deteriorates. Night blindness is among the first signs, and also the earliest ocular symptom of Vitamin A deficiency in children across parts of South and Southeast Asia.
Refractive error is a more common cause than most people expect. An uncorrected prescription produces blurred vision in all conditions, but the effect is amplified at night when the pupil is dilated and optical aberrations are greater. Many people who think they have a structural night vision problem are simply overdue for a prescription update.
Cataracts are among the most frequent causes of poor night vision in adults over 50. The progressive clouding of the lens scatters light, producing glare and haloes at night. Cataract surgery removes the clouded lens and is one of the most reversible causes of night blindness.
Retinitis pigmentosa is a group of inherited retinal disorders in which rod photoreceptors degenerate progressively, typically starting in the mid-periphery. Night blindness is usually the first symptom, appearing in childhood or adolescence, followed by gradual visual field narrowing over the years. RP affects approximately 1 in 4,000 people worldwide.
Glaucoma and other conditions that affect the optic nerve or peripheral retina can also impair night vision, since low-light vision relies heavily on peripheral rod function. Diabetic retinopathy, in advanced stages, can reduce overall retinal sensitivity, including in dim conditions.
Night blindness treatment and what it depends on
Night blindness treatment is cause-specific, which is why an accurate diagnosis comes before any treatment decision.
For Vitamin A deficiency: supplementation under medical supervision is effective and often produces rapid improvement once adequate serum levels are restored. Dietary correction through liver, dairy, eggs, and beta-carotene-rich vegetables suits mild deficiency. Oral supplementation is used in clinical cases, particularly with malabsorption. High-dose self-supplementation is inadvisable -Vitamin A is fat-soluble and toxic in excess.
For refractive error, an updated glasses or contact lens prescription corrects the underlying optical cause. Anti-reflective coatings on lenses specifically reduce glare and light scatter that worsen the night driving experience. This is one of the most common and easily addressable causes of poor night vision.
For cataracts: surgery, when indicated, removes the clouded natural lens and replaces it with an intraocular lens. The improvement in night vision after cataract surgery is often significant. The decision on timing is made with the surgeon based on how much the cataract is functionally affecting daily life.
For retinitis pigmentosa, photoreceptor degeneration cannot currently be reversed. One form caused by a mutation in the RPE65 gene has an approved gene therapy (voretigene neparvovec). Low-vision aids, UV-blocking lenses, and orientation training form the practical management approach for most patients.
When poor night vision needs an eye examination
Night blindness that is mild, stable, and clearly explained by an outdated prescription is not an emergency. But several situations warrant prompt assessment:
- Night vision that has changed noticeably over weeks or months without an obvious explanation
- Night blindness accompanied by any narrowing of peripheral vision or tunnel effect
- Night vision problems in a child, particularly if associated with frequent stumbling or difficulty in dim environments
- Poor night vision, dry eyes, dry skin, or other signs that could suggest a nutritional deficiency
- Glare and haloes at night that are new, particularly in older adults, commonly indicate cataracts
- Night vision problems in someone with a family history of retinitis pigmentosa or inherited retinal disease
An electroretinogram (ERG) measures rod and cone cell responses and can identify functional deficits before structural changes are visible. Dark adaptometry measures how completely the eye adjusts to darkness. These tests are available at specialist centres and are the appropriate investigations when hereditary or structural retinal disease is suspected.
Final thoughts on night blindness causes and treatment
Night blindness is not a single condition. It is a symptom with a range of causes, each pointing toward a different investigation and a different management path. The causes that are correctable -refractive error, Vitamin A deficiency, cataracts -are also among the most common, which makes a proper evaluation worthwhile rather than an overreaction.
ASG Eye Hospital, with centres in Kolkata, Guwahati, Patna, Ahmedabad, and more, assesses night blindness with a full slit-lamp examination, refraction, and dilated fundus evaluation. Where hereditary retinal disease or nutritional deficiency is suspected, ERG, dark adaptometry, and serum Vitamin A testing are arranged.
If you or a family member has noticed a change in low-light vision, a proper eye examination will establish whether the cause is something correctable, something manageable, or something that needs monitoring over time.
FAQs
1. What are the most common night blindness causes?
Vitamin A deficiency, an uncorrected or outdated refractive error, and cataracts are the most frequent and most correctable causes. Retinitis pigmentosa is the most common inherited cause. Glaucoma and diabetic retinopathy can also impair night vision in later stages.
2. What are the typical night blindness symptoms?
Difficulty seeing in dim rooms and poorly lit streets, prolonged adjustment time when moving from bright to dark environments, increased glare from oncoming headlights, and reduced peripheral vision in low light. Progressive narrowing of peripheral vision alongside night blindness is a key warning sign for retinitis pigmentosa.
3. Can night blindness treatment fully restore night vision?
It depends on the cause. Vitamin A deficiency responds well to supplementation, often with significant improvement. Refractive error is corrected with updated glasses. Cataracts are resolved with surgery. Retinitis pigmentosa cannot currently be reversed, though gene therapy is available for one specific genetic form.
4. Is poor night vision always age-related?
No. Age causes a gradual, slow decline in night vision. A noticeable change over weeks or months, or night vision significantly worse than that of peers of the same age, is not a normal ageing effect and should be investigated.
5. Can diet improve night blindness?
Yes, when the cause is Vitamin A deficiency. Carrots, sweet potato, dark leafy greens, liver, eggs, and dairy all provide Vitamin A or beta-carotene. If deficiency is clinical rather than dietary, oral supplementation under medical supervision is needed. Diet does not affect night blindness caused by cataracts, refractive error, or retinitis pigmentosa.